The Exposure of Impacted Canines
What does ‘impacted’ mean?
This means that your tooth has been prevented from coming through correctly by bone, fibrous tissue or another tooth. Canine teeth are some of the last to come through and therefore have more potential to become impacted and fail to reach their correct position within the jaws.
How common are impacted canines?
About 2% of the population have an impacted upper canine usually affecting one side only. Most of these impact towards the roof of the mouth (the ‘palate’) but some impact towards the cheek.
Why does it happen?
A variety of factors can reduce the space available for a canine to come through contributing to it becoming impacted. Often there is already a degree of teeth crowding in the jaws due to a shortage of space. In some cases there is a family history of canines being impacted.
What happens if it is left untreated?
If the canine is left in its impacted position a cystic lesion can develop around the crown of the tooth which can then become infected and also cause damage by putting pressure on the roots of the adjacent teeth.
Treatment for an impacted canine is usually part of a course of orthodontic therapy and so you should seek the advice of your orthodontist regarding your particular circumstances.
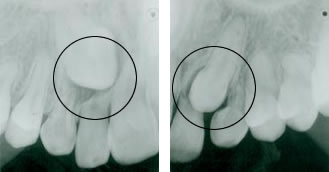
Impacted Upper Canines
Radiographic images of impacted upper canines indicating possible areas of cystic development and root resorption of adjacent teeth.
How will the tooth be exposed?
First x-ray images are used to locate the position of the canine and this will determine whether an “open” or “closed” procedure is required. For both procedures the overlying tissues are surgically raised away from the tooth to allow for sufficient access and appropriate soft tissue and bone removal to expose it.
For an “open exposure” procedure a healing pack is then placed over the tooth to maintain the exposure and non-dissolvable stitches are used to secure this. The pack and stitches are quick and easy to remove and a further appointment will be arranged for this typically 1 week after surgery.
For a “closed exposure” procedure a gold bracket is bonded onto the tooth and the overlying tissue is put back to its original position using fine dissolvable stitches. A gold chain which is already attached to the bracket comes through these tissues and is attached either to an adjacent tooth or alternatively to the orthodontic archwire if braces have already been placed on the teeth.
How long will the operation take?
This depends on the position of the impacted canine and whether the operation is being carried out with local anaesthesia alone or with additional intravenous sedation.
An appointment for surgery under local anaesthesia usually lasts 60 minutes. When intravenous sedation is used an appointment usually lasts 90 minutes; this longer time allows for the recovery period needed before you can be discharged home.
Will I be in pain afterwards?
You should not feel any pain immediately after the operation as the area of surgery will be numb from the local anaesthetic.
As the numbness wears off the area might become uncomfortable and then you should take painkillers. We will supply you with these together with information about doses.
Could there be any after-effects?
This depends on the nature of your operation; if there are any issues in particular to be aware of they will be discussed with you beforehand.
There may be swelling, bruising and discomfort in the area of the surgery. The bruising is usually at its most obvious 2 to 5 days after the procedure and will vary between patients; it normally resolves after 7 to 10 days.
For open exposure procedures, once the pack and stitches have been removed from the area of the exposed tooth the healing usually progresses quite quickly. The stitches used in closed exposure procedures are dissolvable and do not require a further appointment for removal.
We advise that a review appointment is arranged with your orthodontist for 7 to 10 days after your last appointment with us.
When can I return to work?
This depends on your occupation and how you are after your treatment. It may be possible for you to return to college or work the next day but some people will need to take some time off especially if the operation has been carried out under intravenous sedation. We will give you appropriate advice for your particular circumstances.
Postoperative advice
Find out how to help bring about a quick recovery after an operation.
